Diabetic Eye Disease
An overview and treatments for Diabetic Eye Disease.
What is Diabetic Eye Disease?
Diabetes affects the body’s ability to produce insulin or make good use of the insulin it produces, leading to elevated glucose (blood sugar) levels.
Short-term spikes in blood sugar levels can cause intermittent periods of blurry vision or swelling. Persistently high levels of sugar in the blood are more harmful, as they can damage the small blood vessels of the eyes. The blood vessels may swell and leak, or new blood vessels can form and bleed into the eyes. The leaking fluid can scar the ocular structures or cause an increase in the pressure inside the eyes.
If you have diabetes and notice any changes to your vision, The Eye Health Centre team encourages you to reach out to us. We can determine the cause and nature of the eye problem and help manage it, lowering your chances of permanent vision loss.

What are the types and treatments of Diabetic Eye Disease
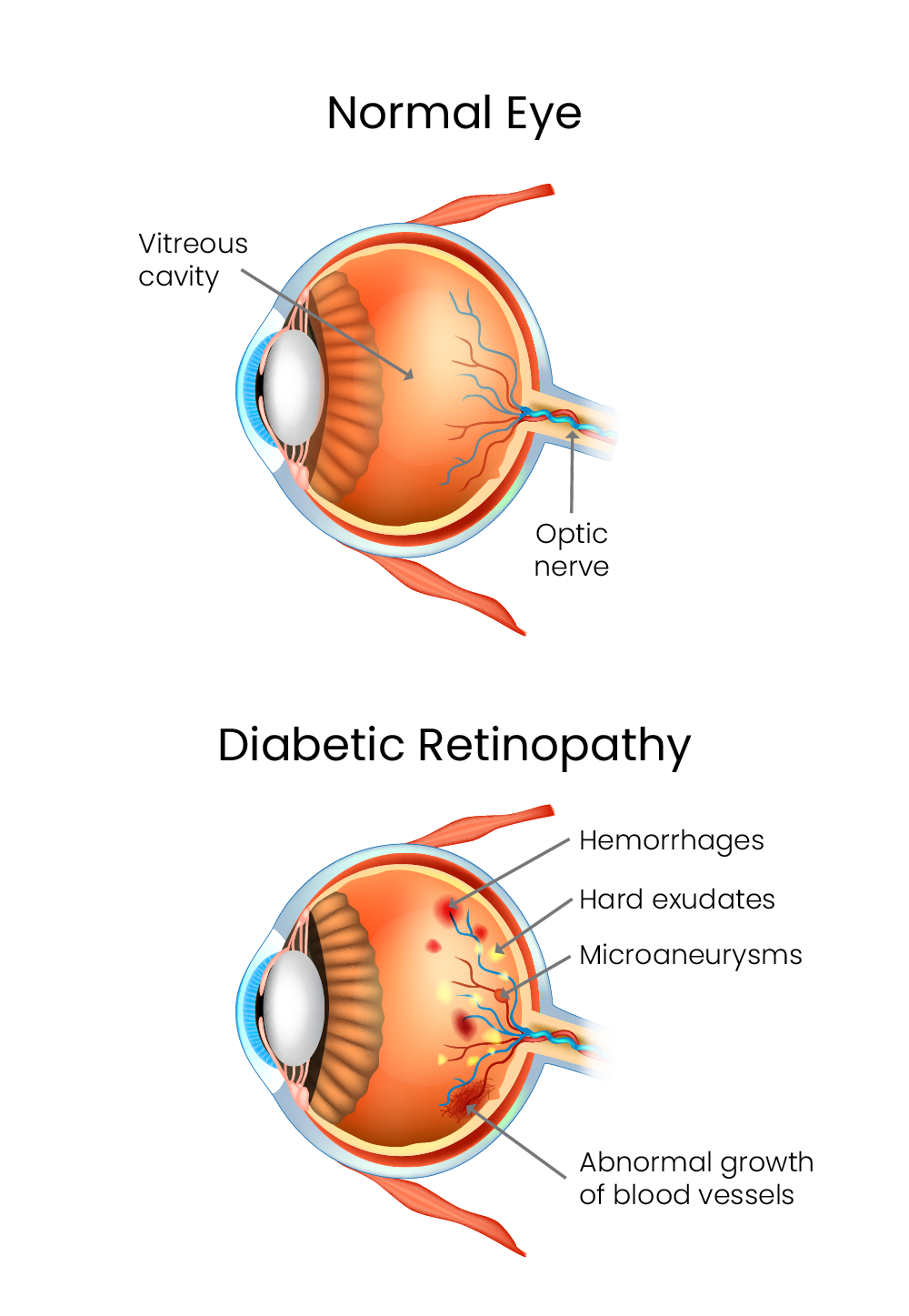
Diabetic Retinopathy and Diabetic Macular Edema
In the early stages of diabetic retinopathy, known as non-proliferative diabetic retinopathy, the blood vessels in the retina weaken, close, swell or leak. In the later stages, known as proliferative diabetic retinopathy, the body responds to the closed-off blood vessels by growing new vessels on the surface of the retina. Unlike normal blood vessels, the new vessels can bleed and fluid and can seriously impair vision.
Treatment for diabetic retinopathy depends on the type and stage of the disease. Our retinal doctors always recommend first getting control of blood sugar and blood pressure levels; that should help promote healthy blood vessels in the eyes. Other treatments include the injection of special medications into the eyes to reduce swelling and slow vision loss, laser surgery to seal off blood vessels and/or vitrectomy to remove blood in the vitreous.
If the fluid leaking from the retina’s blood vessels reaches the macula — the part of the eye responsible for central and detail vision — the macula can swell. This is called macular edema. As a result of the swelling, vision can become blurry or significantly decline.
Glaucoma
People with diabetes are at a higher risk of developing glaucoma, which is often caused by increased levels of pressure inside the eye. Sustained high levels of intraocular pressure eventually damage the optic nerve, or the nerve that transmits information from the eye to the brain.
Although there is no cure for glaucoma, the disease can be treated with the use of medicated eyedrops, laser or traditional surgery or minimally invasive glaucoma surgery (MIGS).
Cataracts
Diabetes also elevates the chances of developing cataracts (a clouding of the eye’s natural lens). There is no non-surgical treatment for cataracts; the eye’s lens must be removed and replaced with an artificial lens. Cataract surgery is very safe and routine.
Early detection and diagnosis of Diabetic Eye Disease
Left undiagnosed and untreated, diabetic eye disease can lead to permanent vision loss and even blindness. But if you have diabetes, you can take steps to reduce your risk of diabetic eye disease. Routine eye exams are strongly encouraged, even in the absence of symptoms.
Optical Coherence Tomography (OCT)
At The Eye Health Centre, we use fluorescein angiography (FA) and optical coherence tomography (OCT) to aid in the diagnosis of diabetic eye disease. With FA, we inject a colored dye into an arm vein and the dye travels through your blood vessels. When it reaches the retina, a camera takes photos of the retina. We then examine the photos to determine whether any blood vessels are leaking or blocked.
With OCT, we use a special machine to scan your retina and provide detailed cross-sectional images of its structures. This assists us in finding and measuring any macular swelling.
Do you have a question or concern about your eye health? To discuss your condition with an experienced ophthalmologist or optometrist, please contact The Eye Health Centre

